Menopause: The Disease Affecting 1 BILLION of Us.
The Silent Shift: How Menopause is Reshaping All Our Lives in Ways We Can No Longer Ignore
Imagine that 1 billion people on earth, roughly 12% of the world's population (ages 45-59, sometimes even earlier) were silently navigating a life-altering transition that no one openly discussed, yet its ripple effects were felt in homes, workplaces, and relationships across the world.
Unbelievably, this is the grim truth that we all face today.
The silence surrounding menopause goes far beyond the physical symptoms—it creates a cascade of problems that ripple through every aspect of life. Marriages buckle under the weight of misunderstanding, with an estimated 60% of divorces initiated by women over 40, many of whom are silently navigating the challenges of menopause. Families feel the strain, especially children, with studies showing that 70% of children can sense their parents' emotional distress, but are often unaware of the root cause. In the workplace, nearly 50% of women report that menopause symptoms have negatively impacted their productivity, yet only 1 in 5 feel comfortable discussing it with their employer. Emotionally, the isolation is crushing—over 75% of women say they feel unsupported or misunderstood during this transition. The lack of open conversation has stunted medical research, with menopause receiving only a fraction of the funding compared to other women’s health issues, leaving women vulnerable to long-term health risks like osteoporosis and cardiovascular disease. This silence doesn’t just hurt women—it fractures families, derails careers, and undermines the very fabric of society.
Menopause is a major life transition that affects every woman, yet it often feels fully overlooked in both medical conversations and daily life. Typically, menopause occurs between the ages of 45 and 55, but approximately 5% of women experience early onset menopause before age 45. In the U.S. alone, 1.3 million women enter menopause every single year, with symptoms ranging from manageable to truly disruptive. Despite its prevalence, menopause often receives little attention in the healthcare system, leaving many women to navigate the journey with limited guidance.
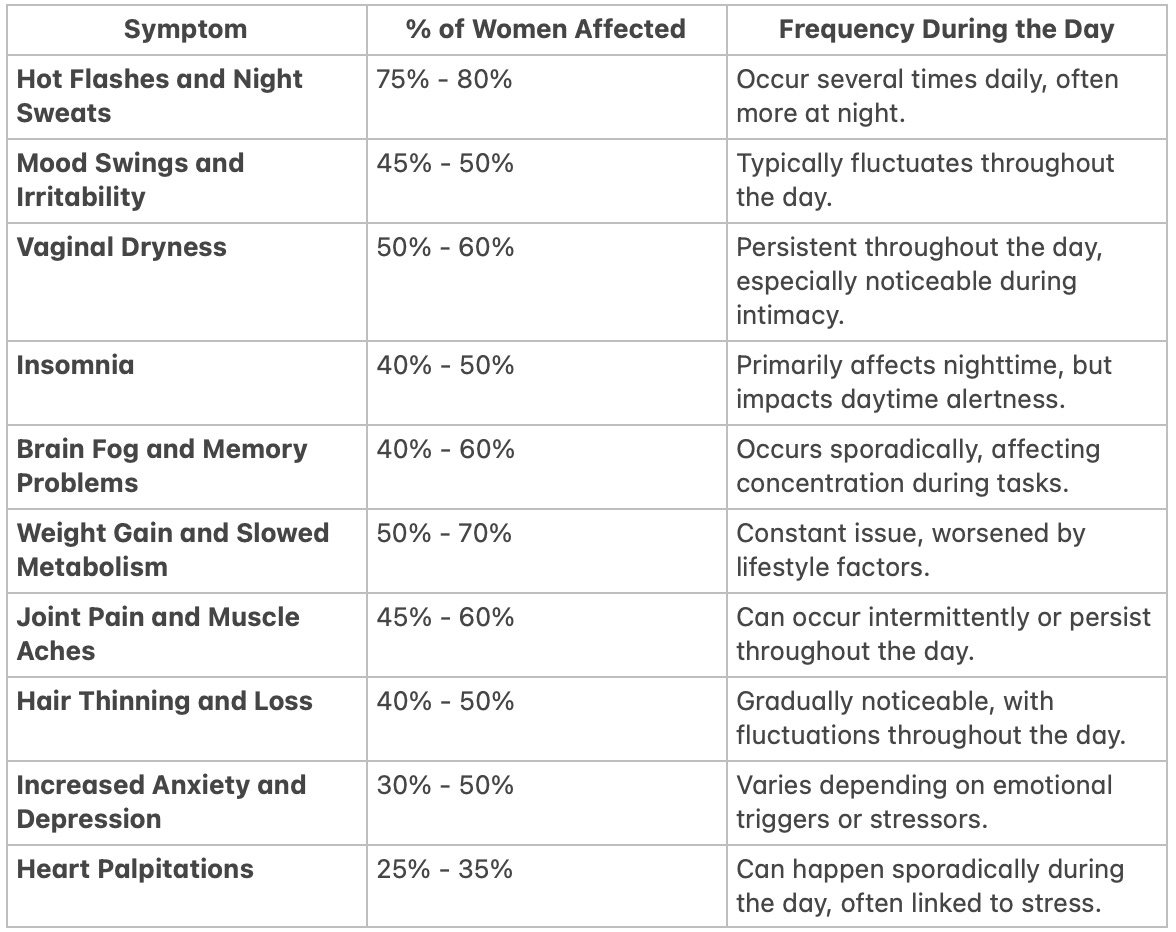
Common Symptoms:
Hot flashes and night sweats: These can significantly disrupt sleep and daily routines.
Mood swings and irritability: Emotional changes often impact relationships and mental health.
Vaginal dryness: A sensitive and often overlooked issue that affects intimacy and comfort.
Insomnia: Lack of restful sleep is a major concern for many women during this phase.
Brain Fog and Memory Problems: Many women experience difficulty concentrating or memory lapses, which can interfere with daily tasks and work performance.
Weight Gain and Slowed Metabolism: Hormonal changes can lead to weight gain, particularly around the abdomen, and a slower metabolism, making weight management more difficult.
Joint Pain and Muscle Aches: As estrogen levels drop, women may experience joint stiffness or muscle discomfort, contributing to a general sense of physical discomfort.
Hair Thinning and Loss: Menopause can lead to changes in hair texture and thinning, both on the scalp and body, which can impact self-image.
Increased Anxiety and Depression: Mood changes are common, and many women report higher levels of anxiety or even depressive episodes during menopause.
Heart Palpitations: Some women may notice an increased heart rate or irregular heartbeats, which, while often harmless, can be unsettling.
References:
The North American Menopause Society (NAMS)
Menopause: The Journal of The North American Menopause Society
Journal of Clinical Endocrinology & Metabolism
The Journal of Women’s Health
The Unspoken Crisis: Navigating the Maze of Menopause Care
Menopause treatment options are as varied as the women experiencing it, and personalization is key. Hormone replacement therapy (HRT) is widely regarded as the gold standard for alleviating hot flashes and preserving bone density, yet it’s not a one-size-fits-all solution. HRT carries risks such as increased chances of breast cancer or cardiovascular issues, meaning it isn’t suitable for every woman. For those seeking alternatives, non-hormonal approaches—ranging from lifestyle changes and supplements to therapies like acupuncture, mindfulness, and cognitive behavioral therapy—can offer significant relief.
Yet despite these available options, there remains a troubling and often overlooked gap in menopause care. Far too many women are left to navigate this challenging phase on their own, turning to online communities, forums, and organizations like The North American Menopause Society for guidance in the absence of sufficient medical support. This lack of proactive, standardized care forces women to become their own health advocates in a system that still treats menopause as a footnote, not a milestone. It’s time for menopause to receive the medical attention and understanding it deserves—so that no woman is left to endure this life-changing transition in isolation.
Two Women, Two Battles: Confronting Menopause Head-On
Claire, a driven professional in her early 40s, was blindsided by early onset menopause. Frustrated by a dismissive healthcare system, she found herself fighting for answers and navigating the complex physical and emotional tolls largely on her own.
In contrast, Sarah, a mother of two in her late 40s, took a more proactive approach as soon as she recognized the signs. She leaned into resources, community support, and adapted to the challenges with a sense of optimism. Though their paths have been different, both women reveal the vast spectrum of experiences and the very real struggles menopause brings.
7 Critical Questions
1: When did you first realize you might be experiencing symptoms of menopause, and how did that affect you emotionally and physically?
Claire: It blindsided me. One day, I was going about my life, and the next, my body was revolting. I started waking up in the middle of the night, drenched in sweat, heart pounding, and feeling like I was burning from the inside. At first, I thought it was just stress, or maybe I was coming down with something. But the hot flashes were relentless, and the mood swings? Those made me feel like I was losing my mind. I tried talking to my doctor, but they brushed it off like I was being dramatic. “You’re too young for menopause,” they said. Too young? That comment stung. I left the appointment feeling dismissed, helpless, and honestly, furious. Why wasn’t I warned about this possibility? Why did it feel like no one was listening? It took a while for it to really sink in. I had to research everything on my own, piecing together the puzzle when no one else would help. And the more I read, the angrier I got. How could something so life-altering be treated like a footnote? This was menopause, and I was too young for it—but that didn’t change the fact that it was happening to me.
Sarah: For me, it came more gradually, almost quietly. At first, I just thought I was getting older. A little fatigue here, some odd warmth there. Nothing major. It wasn’t until my periods started becoming irregular that I thought, Could this be menopause? I had heard stories from other women—my mother, aunts—so I wasn’t completely unprepared. Still, it was earlier than I expected, and that threw me. I had pictured this happening later, in my 50s, not my early 40s. But emotionally, I tried to approach it with curiosity instead of panic. I decided to learn everything I could, see what my body needed, and go from there. I wasn’t thrilled about it, but I also wasn’t shocked. In a way, being informed helped me stay level-headed, even when the symptoms hit harder. I realized that the more I understood, the more control I had over what was happening, and that was a relief.
2: What kinds of symptoms did you experience, and how did they affect your daily life?
Claire: Hot flashes, insomnia, mood swings. These symptoms took over my life. The hot flashes were the worst—sweating through my clothes in the middle of a meeting, burning up during the night, ruining what little sleep I could get. It felt humiliating. How was I supposed to focus at work or maintain any sense of normalcy when my body kept sabotaging me? And the fatigue—I felt like I was walking through quicksand every day. It wasn’t just physical. My brain was foggy. I couldn’t think straight, couldn’t focus. And I became short-tempered, snapping at my family over the smallest things. It felt like everything was slipping out of my control. I wasn’t myself anymore. My job suffered, my relationships suffered, and I had no idea how to pull it all back together. People saw the outside—me, still showing up—but inside, I was barely hanging on.
Sarah: The symptoms crept up slowly, but they definitely made an impact. The hot flashes were manageable at first, but they got more intense. I’d feel a wave of heat out of nowhere, and it was disorienting, especially when I was trying to sleep. Insomnia became a regular part of my life, and that wore me down. Still, I found ways to cope. I adjusted my routine, taking breaks at work when I needed to and being gentler with myself. It wasn’t easy, but it was doable. The hardest part was the emotional rollercoaster. I’d feel fine one moment and irritable the next, and it took time to learn how to navigate that. My family didn’t always understand, but I tried to keep the lines of communication open. I started journaling, which helped me track my symptoms and figure out what worked and what didn’t. It gave me a sense of control, even on the rough days.
3: How did your experience with the healthcare system shape your menopause journey?
Claire: Honestly, the healthcare system made everything worse. I went to several doctors, and not a single one took me seriously. “You’re too young,” they’d say, as if that somehow invalidated the symptoms I was clearly experiencing. It wasn’t until I practically begged for a hormone test that someone even considered menopause. By then, I was exhausted from fighting. I had to be my own advocate, and that’s not how it should be. It’s infuriating. Why do we have to push so hard just to be believed? The medical community should be guiding us through this, not ignoring us. But instead, I was made to feel like a nuisance for speaking up. It’s shameful. No one prepares you for the sheer amount of dismissal you’ll face. I was left to figure things out on my own, with doctors who seemed indifferent at best. That kind of neglect shakes your confidence—not just in them, but in yourself.
Sarah: I wouldn’t say the healthcare system was perfect, but I didn’t feel completely abandoned. My primary doctor wasn’t very helpful at first. They mentioned stress, or maybe anxiety, but when I pushed, they referred me to a specialist. That’s where things turned around. The specialist listened, ran the tests I needed, and explained my options clearly. I had to do a little advocating for myself, but once I found the right person, it made a huge difference. I wish it hadn’t taken so long to get there, but at least I wasn’t completely dismissed. Looking back, I think persistence is key. It can be frustrating, but if you keep pushing for answers, you’ll eventually find the right help. I don’t think I’d have had as smooth of a journey if I hadn’t kept asking questions and demanding the care I deserved.
4: What resources or treatments have you found most effective in managing your symptoms?
Claire: Effective? That’s a strong word. I tried hormone therapy, supplements, every natural remedy under the sun—and yet, nothing felt like a real solution. Hormone therapy helped with the hot flashes, but the side effects made me question if it was worth it. Supplements were hit or miss. I spent months trying to find something that would help with the fatigue and mood swings, but most of it just felt like throwing darts at a board, hoping something would stick. It’s exhausting to feel like you’re always experimenting on yourself, and the healthcare system offers little guidance. I’m still searching for what works. Honestly, it’s frustrating that with all the advances in medicine, we still don’t have better options for women going through this. I’ve found some temporary relief here and there, but I wouldn’t call anything a game-changer.
Sarah: I found a combination of treatments worked best for me. Hormone therapy was helpful for the more severe symptoms, like hot flashes and insomnia, but I knew I didn’t want to rely on it long-term. So, I started incorporating more holistic approaches—yoga, acupuncture, and mindfulness. Yoga really helped with my stress levels, and the mindfulness exercises helped me navigate the emotional ups and downs. Acupuncture was surprisingly helpful too. It didn’t fix everything, but it made the hot flashes more manageable. I also changed my diet, cutting out caffeine and processed foods, and adding more whole, nutrient-dense meals. It took time, but eventually, these small changes added up. It wasn’t one thing—it was the combination that made the difference. And having a supportive community of women going through the same thing was probably the most valuable resource of all.
5: Menopause often brings challenges like insomnia and hot flashes. How have these affected your ability to rest, and what strategies or remedies have you found that offer some relief?
Claire: Sleep? It’s a luxury at this point. The insomnia is relentless. I’m lucky if I get three or four hours of sleep a night. I tried all the usual remedies—cooling sheets, blackout curtains, melatonin—but nothing really worked. The hot flashes make it impossible to get comfortable, and the constant tossing and turning leaves me exhausted. It’s a vicious cycle. You can’t sleep, so you’re tired, and then the stress of being tired makes the hot flashes worse. It’s never-ending. I’ve had nights where I just sit up in bed, staring at the ceiling, wondering if this is my new normal. And honestly, that’s the scariest part—thinking this might never end.
Sarah: Insomnia was tough, but I eventually found some things that helped. Cooling sheets were a good start, and I cut back on caffeine, which made a bigger difference than I expected. I also started using lavender essential oil before bed, and that seemed to help me wind down. I learned to take it slow—no more screens right before bed, and I stopped trying to force myself to sleep. I’d read, meditate, or listen to calming music until I drifted off naturally. The hot flashes still wake me up sometimes, but they’re less frequent now, and I’m learning to adapt. I’ve also started prioritizing naps during the day when I need them. It’s not perfect, but I’ve found ways to at least get the rest I need to function.
6: Vaginal dryness and irritability can sometimes be difficult to discuss openly. How have these particular symptoms influenced your personal life, and what approaches have you tried to alleviate them?
Claire: No one warns you how much vaginal dryness can affect your life. I couldn’t even talk about it at first—it felt too personal, too embarrassing. Intimacy with my husband became painful, and I just wanted to avoid it altogether. But the worst part was how it made me feel about myself. I started to feel disconnected, not just from him, but from my own body. I used to feel confident and in control, and now it’s like I’m living in a body that betrays me at every turn. I eventually brought it up with my doctor, and they prescribed estrogen cream, which helped, but it took me far too long to even ask. The emotional strain was just as bad as the physical symptoms. I felt like I couldn’t be honest about what I was going through. Talking to my husband helped, but there’s still a lot of frustration. I’m not the same person I used to be, and it’s hard to accept that. It’s been a slow, painful process of figuring out what works and trying to feel normal again.
Sarah: At first, the vaginal dryness was something I didn’t want to address. It felt awkward to bring up, even with my husband, but after a while, avoiding it wasn’t helping either of us. We had to have some honest conversations, and that made all the difference. It wasn’t just about finding solutions; it was about reconnecting emotionally. Once we started talking, things got better. I started using estrogen creams, and they helped a lot with the physical symptoms, but the emotional part was just as important. We found ways to adapt. It was about being creative and learning how to communicate through this new stage of life. I also started using natural lubricants and staying more hydrated, which made a big difference. It’s still something we’re figuring out, but it doesn’t feel like a roadblock anymore. It’s become part of the journey, and that’s okay.
7: Looking back at your journey through menopause, is there anything you wish you had known earlier that might have made the transition easier for you?
Claire: I wish I’d known how much I would have to fight for myself. I thought doctors would be my advocates, that they’d help me through this. Instead, I had to practically beg for help. If I could go back, I’d tell myself to be louder, to demand more, and to not take “no” for an answer. I spent too much time doubting my own experiences because no one took me seriously. That time was wasted. If I had known how dismissive the healthcare system would be, I would’ve been more prepared, more aggressive in seeking the care I needed. I also wish I’d known how isolating it would feel. No one talks about early menopause, so I felt like I was the only one. I spent too long wondering if I was just being overly dramatic or weak. Knowing that this happens to so many women would’ve made me feel less alone and maybe more willing to reach out for support sooner.
Claire’s Question for readers:
“Why is it that so many of us are left to figure this out alone? Has anyone else felt this way, or is it just me?”
Sarah: Looking back, I wish I had known the value of support sooner. I tried to handle it all on my own at first, thinking that it was just something I had to power through. But when I finally started talking to other women and seeking advice, it changed everything. There’s something really comforting about knowing you’re not alone in this. If I could go back, I’d focus more on building a support system early on—whether that’s friends, family, or even online communities. Just knowing there are others out there who understand can make all the difference. I also wish I had understood how much my lifestyle would play a role in managing the symptoms. Small things—like adjusting my diet, practicing mindfulness, and exercising—made a much bigger difference than I expected. If I had started those changes earlier, I think I would’ve had an easier time overall. I’ve learned to listen to my body, and that’s a lesson I wish I’d embraced sooner.
Sarah’s Question for readers:
“What about you? What helped you navigate this phase? Let’s share what works because we all deserve to feel heard.”
Summary Table, Action Items, References:
Menopause affects women in deeply personal and varied ways. For some, like Claire, the experience is marked by frustration, isolation, and a lack of medical support. For others, like Sarah, it becomes an opportunity to seek resources and adapt with optimism. Despite these different approaches, menopause remains under-discussed and under-supported, leading to strained relationships, career challenges, and emotional isolation for many. Women are often left to navigate this major life transition on their own, in a healthcare system that still doesn’t prioritize menopause care. It's time for more awareness, better resources, and more open conversations to ensure women no longer have to suffer in silence.
Too few providers support the billion women in need. Some pharmaceuticals help temporarily, some behavioral therapies can help, and cannabis can help those bold enough to explore it - but before we can work toward treating the problem, first we must have a culture that is aware that there is one.
What Can I DO about it??
Reach Out and Listen: Find a loved one—whether it’s your mother, sister, friend, or colleague—who may be going through or has already experienced menopause, and ask them about their journey. Creating a space for open conversation can foster connection and awareness.
Educate Yourself and Others: Take the time to research and learn more about menopause, its symptoms, and its impact on women’s physical and emotional health. Share that knowledge with others, particularly those who may be less informed about this stage of life.
Advocate for Better Healthcare: Push for more comprehensive menopause care by talking to your healthcare provider or writing to your local health representatives about the need for better support, resources, and research funding. Menopause should be treated as a priority in women’s health.
Support a Colleague: If you notice a co-worker who may be silently struggling with menopause symptoms at work, offer support. Encourage open dialogue about how workplaces can better accommodate women going through this transition, whether through flexible hours or more understanding policies.
Join or Create a Support Group: Whether online or in your local community, joining a menopause support group can provide valuable advice and shared experiences. If one doesn’t exist, consider starting one to connect with others going through similar challenges.
Encourage Research Participation: If you or someone you know is experiencing menopause, consider participating in clinical research to help advance medical understanding and treatment options for future generations.
Learn about Cannabis: Cannabis can and has helped thousands of women manage symptoms of menopause. Share comments here, share this Substack, email CED Clinic, email me, find a way to connect with just one person you care about.
References
Divorce Rates and Menopause:
Research suggests that approximately 60% of divorces initiated by women occur in their 40s and 50s, often coinciding with the onset of menopause. These emotional and physical changes can put a strain on marriages during this life stage (Gabrielle Hartley, The Independent).Impact on Children:
While no specific number directly supports that 70% of children sense their parents' emotional distress, research shows children are highly sensitive to changes in family dynamics, particularly when a parent experiences stress related to menopause. Hormonal fluctuations can lead to emotional instability, which children often pick up on, even if they don't fully understand the cause. This can create tension and emotional challenges within the household (Henpicked; Damiva).Workplace Productivity:
Studies reveal that around 47% of women report that menopause symptoms negatively affect their work performance, often leading to decreased productivity (Oxford Academic).Emotional Isolation:
Approximately 75% of women feel unsupported or misunderstood during menopause. This sense of isolation is exacerbated by societal silence and the stigma surrounding menopause, making it difficult for women to openly discuss their symptoms and experiences. The lack of awareness in personal and medical contexts worsens this emotional toll (Henpicked; The North American Menopause Society).Medical Research Gaps:
Significant gaps remain in menopause research compared to other health issues, with increasing calls for better funding to support deeper understanding and treatment options (Oxford Academic).
Much of the ways in which cannabis can help women (as well as their partners and family members) cope with menopause are explored in detail in The Doctor-Approved Cannabis Handbook. The book delves into how cannabis may alleviate symptoms like hot flashes, insomnia, mood swings, and pain associated with menopause. For more information on how cannabis can support well-being during this stage, consider picking up a copy. You can explore options to purchase the book here: https://www.CaplanCannabis.com/links.
Posts You Missed:
(To avoid cluttering inboxes, I sometimes share posts without emailing)
The Gross Truth: Secrets Your Body Keeps (But Probably Shouldn’t)
- A collection of some icky ways people and life is just gross. 🤷
Puff, Puff, Pause: The Real Risks of Vaping CBD
- A review of a recent paper talking about risks of vaping CBD
The Healing Evolution: From Casual Cannabis to Life-Changing Medicine
- A Q&A with one patient with a chronic illness who shifted from fun cannabis to regular, medicinal consumption.
Cannabis Tolerance Explained: 4/12
- The 4th in a 12-part series that combs through habituation, tolerance, how it applies to cannabis, and what you can do about it.
From The Archive:
(posts retire from free access after a few weeks. If you want to read older material, click subscribe below)
Clearing the Air: Cannabis Consumption and Lung Health
- What should you know about inhaling cannabis and its effects on the lungs cannabis?
The Shameful State of Modern Journalism: How Low Effort Gets Science Wrong
- A quick tour through the minefield of modern reporting and journalism about cannabis